It is 8 o´clock in the morning and it is an ordinary day at “the office” for Ph.D., Associate Professor and MD Mette Munk Lauridsen and Ph.D. Charlotte W. Wernberg from the Danish National Research Foundation´s Center of Excellence, Center for Functional Genomics and Tissue Plasticity, (ATLAS).
The project nurse, Lea L. Grønkjær has arrived half an hour earlier, to get ready for today´s biopsy.
The Liver outpatient clinic 242, on Hospital of South West Jutland in Esbjerg, room 13 is now ready, and at a quarter past eight, Lea welcomes the first test person of the day. The patient is a 43-year-old female. She comes in for her first visit in the study. In this project, her first and last visit is 2.5 years apart. Also, that she is a woman is not a coincident, since 73% of the test persons are female.
Getting ready
The first approximately 45 minutes is the preparation of the patient. Lea does many different tests: weights and measures the patient, and does two cognitive brain tests. The latter is to examine if the patient has liver-conditioned brain disturbance (hepatic encephalopathy).
Finally, Lea controls the amount of fat and stiffness in the liver using a specialized scanner. The patient is now ready for liver biopsy.
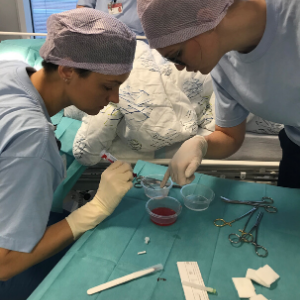
The atmosphere in the room is good. The patient seems very calm, as she lays in the hospital bed, getting ready for her biopsy. The intervention itself is over in about 10 minutes. MD Mette Munk Lauridsen removes a small amount of adipose tissue and takes a liver biopsy under local anesthesia, and hand it over to Ph.D. Charlotte W. Wernberg who prepares the samples for transport to Odense and subsequent analyses. One senses that they have done it before. The work is done quickly and professionally so the samples can be frozen as soon as possible. The biopsies will be used for transcriptomics (including single cell transcriptomics) and proteomics analyses to provide insight into human adipose (fat) and liver tissue plasticity during regression of obesity in response to bariatric surgery.
When it is all over the patient must wait in an observation room at the hospital for a minimum of four hours before going home. The patient tells me, that this is the hardest part, just waiting for hours.
Luckily, I can see in her purse that she has her knitting and an iPad to keep her entertained.
To be a part of the project you need to be obese, which means a body mass index over 35. Both the MD and the nurse in this project are in a clinical research position, so they use 2 days a week for patients and the rest for preparation, office work and research. The Ph.D. Student work full time on the project. In busy weeks, they see about 5 patients. For now, the project has 100 included participants. To keep track of it all, a secretary helps for a few hours a week, with booking the planned follow-up visits.
Mette, Charlotte and Lea do everything in the patient inclusion process. No job in the project is too small for them, and they are all very hands-on!
Preparation – The PROMETHEUS protocol
To reach this far, several years of preparation have gone by. Mette has worked on the project preparation since the summer of 2017 in a postdoc position. By mid-2018, The Kragh research Group from ATLAS obtained ethical approval of the PROMETHEUS protocol and the team from today’s biopsy at Hospital of South West Jutland in Esbjerg got permission to perform clinical sampling of liver (hepatic) and fat (adipose) tissue from obese patients undergoing bariatric surgery.
What does the project give back to the test persons?
All the test persons get a thorough metabolic health check plus a focused cognitive and mental check-up.
Also if they show signs of:
Severe liver fibrosis – Then they get a clinical follow-up.
-Pre-diabetes, high blood pressure or cholesterol – referral to GP for follow-up.
-Sleep apnea – referral for diagnostic workup.
-Food addiction and depression – guidance towards psychologist.
And at all controls – They get guidance towards municipally available diet counseling.
For more information:
www.sydvestjysksygehus.dk
www.sdu.dk/en/flash
dg.dk/en/
COVID-19
Like every Hospital in Denmark during this time, things have changed.
Room 13 at the Liver outpatient clinic 242 has now been transformed into extra intensive spaces, like the rest of the ambulatorium.
For now they take one day at a time, and try to follow up on the most important visits in the study.
Some visits will be postponed.
For more information, please contact Charlotte